Data Analytics Can Address the U.S. Substance Abuse Crisis
Lifecycle Management & Modernization, Data & Analytics, Health, Health Policy Transformation, Healthcare Management, Health Security, Logistics, Performance OptimizationSubstance abuse is on the rise in America, but the federal government has an opportunity to leverage data analytics for an effective response.
More than 20 million people in America have a substance abuse disorder. As rates of substance abuse in America rise, prevention and treatment are a growing priority for the federal government.
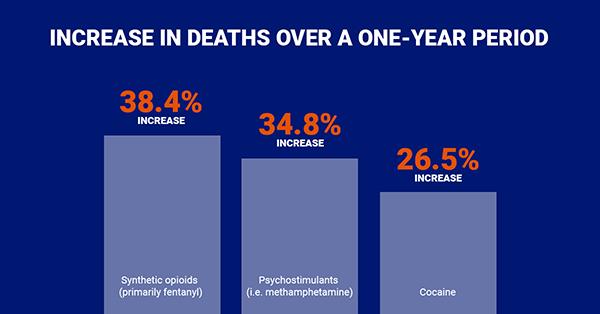
The COVID-19 pandemic has deeply aggravated the problem, putting additional pressure on federal stakeholders to craft a comprehensive response plan. Preliminary data from 2020 suggest that substance abuse of all types worsened when lockdown policies were implemented, as many were forced to spend months in triggering environments without the support networks they had prior to the pandemic. Opioid addiction rates, for example, are reaching new highs. A new Princeton University study suggests that in addition to isolation, COVID-19 limited access to opioid dependency treatment. As a result, emergency rooms around the country are triaging not only COVID-19 patients but those experiencing overdose or other substance abuse-related issues at higher rates than before. According to data from the Centers for Disease Control and Prevention, the United States recorded 81,000 drug overdose deaths from June 2019 to May 2020, its highest ever in a 12-month period.
Fortunately, the federal government has made strides in data collection and monitoring, lending new insights into the fields of non-addictive pain management and prevention services such as monitoring systems to guard against overprescription. In this article, LMI experts offer insights into how federal stakeholders can leverage what’s available to improve public health outcomes.
Use Data To Identify Broad Trends—and Outliers
In 2018, Congress passed the SUPPORT for Patients and Communities Act, which paved the way for improved data collection and integration across the federal healthcare landscape. Monitoring systems that previously could not communicate with each other now have the authorization and funding to do so. Insurers and law enforcement agencies have used these new capabilities to stop egregious cases of overprescribing in addition to identifying fraud, waste, and abuse.
“Once you start collecting and unifying data, there is an opportunity to use analytics not just to identify broad trends but also to drill down and investigate outliers,” explains Jordan Leach, a data analytics consultant with LMI.
Leach notes that as federal- and state-level stakeholders gain a clearer perspective through integrated substance abuse data—both nationally and in their communities—they can formulate better response plans. The data can be used to gain buy-in within agencies by showing the cost and scope of the problem and the efficacy of any given response.
"Once you start collecting and unifying data, there is an opportunity to use analytics not just to identify broad trends but also to drill down and investigate outliers.”
Combine Analytics and Subject Matter Experts to Uncover Nuance in Data
A common feature of opioid addiction is dependency due to chronic pain. The challenge with treating substance abuse—especially substances legitimately prescribed by doctors—is that cutting the supply worsens the problem. Without a prescription, some opioid users switch to far more dangerous heroin or fentanyl obtained on the black market. In addition, individuals with legitimate needs could find themselves without effective solutions.
Through analysis and modeling, federal- and state-level stakeholders can identify key insights that build flexibility into health systems and policy, ultimately making them more impactful and cost-effective. Analyzing data for availability of medication-assisted treatment as well as addressing social determinants of health such as homelessness, lack of transportation, and joblessness can highlight effective evidence-based practices in combating the opioid crisis. These capabilities, paired with subject matter expertise, can identify suspect prescribing activity as deviations from what’s anticipated based on history, source, the prevalence of risk factors, and other contexts. For example, a large number of prescriptions from a chronic pain clinic in a high-need area might be considered normal, while the same or even a smaller number from an individual physician could signal overprescribing. Nuanced analysis of multiple variables helps ensure that pain clinic patients aren’t cut off from medically necessary treatments.
Leverage Science for Effective Alternatives and Data To Track Their Adoption
Federally funded research and development can accelerate new opioid-alternative treatments and demonstrate their effectiveness. The National Institutes of Health, for example, launched the Helping to End Addiction Long-term (HEAL) Initiative in 2018 as a cross-agency effort that has since funded more than 70 clinical research projects for pain management. The Chronic Pain Management Research Program, part of the Department of Defense’s Congressionally Directed Medical Research Programs, awarded $13.3 million last year to 10 research projects aimed at producing effective interventions for military service members and veterans living with chronic pain.
The rigorous scientific evidence derived from such efforts can help insurers incentivize physicians to implement alternative treatments with similar or greater effectiveness. Medicare, for example, recently approved the use of acupuncture for management of chronic lower back pain. This decision was based on decades of scientific research showing its efficacy, and it has embedded new flexibility into the healthcare system. With this change, providers have another approved tool for treating pain without risk of addiction. With analysis of Medicare claims data, government stakeholders can gain additional insight into how, where, and when this tool is being used.
Protect Privacy by Creating Synthetic Populations
Patient privacy laws can make it difficult to understand the scope of substance abuse nationwide. Historically, some individuals have abused this privacy to fill prescriptions multiple times from different providers or pharmacies. Where monitoring systems are in place to track prescription fulfillments and purchases of controlled substances, data often hasn’t been shared between systems or with law enforcement, sometimes because of federally protected health information. Even then, there are no monitoring systems to track individual purchases of alcohol, tobacco, and illegal drugs.
Artificial intelligence paired with data analytics can alleviate privacy concerns by creating anonymized synthetic populations. These representative population samples are based on aggregate data parsed by artificial intelligence. They retain the information pertinent to addiction and treatment but mask any trackable link to an individual. Synthetic population data don’t carry the same privacy limitations as the personally identifiable health data of real individuals. They can help national and local governments understand the scope and trend of problems within specified communities and the effectiveness of targeted policy and programs.
Synthetic populations have been used to model programs such as needle exchanges and providing rapid detoxification drugs (such as naloxone, or Narcan) to community organizations. Successful modeling can help stakeholders understand an intervention program’s potential cost savings and impact on health outcomes, often the first crucial step in launching a pilot demonstration.
Save Lives via a Coordinated Federal Response
Although substance abuse is growing at unprecedented rates in the United States, there are more tools, funding sources, and data to prevent and treat it. Leveraging analytics to understand the scope and scale of the problem as well as identifying alternative treatments will go far toward improving public health. Analysis of new trends in alternative pain management, for example, can further support hard-to-reach populations and reduce the cost of care. Opioid addiction treatment is not a one-size-fits-all proposition. Care is enhanced when population health, predisposition to addiction, and available resources are addressed in ways that are realistic, patient centered, and data driven. A coordinated federal response that embraces data and supports proven practices and technologies will encourage a faster end to this crisis, saving federal taxpayers billions each year and promoting a more equitable and effective healthcare system.
LMI has more than two decades of experience analyzing diverse healthcare data to inform health program and policy improvements. We work at the intersection of science, policy, logistics, and analytics to facilitate innovation in healthcare provision and payment, implement federal healthcare priorities, advance health security, and optimize service delivery and program effectiveness.